This website uses cookies to enhance the user experience. By using Yoppie you are agreeing to our use of cookies.

Contraception & Your Cycle
The enormous range of contraceptive options out there can be overwhelming; we discuss all the varieties available and how they impact your menstrual cycle.
Where to get contraceptives for free
What's the difference between hormonal and non-hormonal?
Hormonal contraception
The combination pill or combined contraceptive pill
The progestogen-only pill / "mini pill"
The hormonal intrauterine system IUS (the hormonal coil)
The 3-month shot / contraceptive injection
The implant
The patch
The vaginal ring (the NuvaRing)
Emergency contraceptive (the “morning after” pill)
Non hormonal contraceptives
Intrauterine device IUD / "copper coil"
Condoms (for men)
Condoms (for women)
Cervical cap or diaphragm
Pull out method
Rhythm method, with temperature monitoring
Key takeaways
Access to reliable contraception has transformed the lives of women all over the world - giving us more control and choice over how we live our lives. But as there’s so many options available, choosing which contraception to use can seem like a bit of a minefield!
After a while, most of us get pretty used to our cycle and what’s normal for us. But starting or switching contraceptives can have us back at square one again when it comes to knowing what to expect from our periods. This can be annoying, but it’s ok to switch contraceptive methods until you find one that you’re happy with, that works for you and your body.
You’ve probably heard a few horror or success stories from friends about certain kinds of contraception! This will have possibly already shaped your view on which methods you’d be happy to try. But we’re all different, so it’s good to keep an open mind. Not everyone will have the same experience using the same type of contraception, as you’ll see from quotes we’ve included from women all over the UK about their own experiences.
After researching different methods, before deciding, speak with your GP or sexual health clinic. Once you’re trying a new form of contraception, listen to your body and pay attention to any changes. If you feel it’s not the right choice for you, it’s ok to stop and try something different.
There are all kinds of factors to take into consideration when choosing contraception, including age, lifestyle, medical history, potential plans for future pregnancies, and current medication. But ultimately, it’s your decision! In this guide, Yoppie delve into all contraception methods - hormone and hormone free - focusing on how they might affect your cycle and fit in with your lifestyle. So, if you’re feeling confused about what contraception could be right for you, read on! What we’re covering in this article is
Hormonal contraception including:
- The combination pill
- The progesterone only pill (sometimes called the mini-pill)
- The hormonal Intrauterine system IUS (the hormonal coil)
- The 3-month shot
- The implant
- The patch
- The ring
- Emergency contraceptives
Non hormonal contraceptives including:
- Intrauterine device IUD (sometimes called the copper coil)
- Condoms
- Diaphragm
- Cervical cap
- Pull out method
- Rhythm method with temperature monitoring
Where to get contraceptives for free
Almost all forms of contraception covered here are available for free from the NHS. Your local GP, sexual health clinics (GUM clinics) and some young people’s services should be able to help you organise an appointment to discuss your options and begin a new form of contraception.
If you want to try less popular methods like the female condom, for example, they are not always available from all contraception, doctors or sexual health clinics so you may need to call ahead to check.
What's the difference between hormonal and non-hormonal?
Hormonal contraceptives use synthetic hormones to prevent pregnancy, and non-hormonal methods tend to stop sperm entering the uterus by introducing physical barriers. Both types of contraception are effective, and there are pros and cons to both.
Let’s dive in and look at the options in more detail…
Hormonal contraception
Hormonal contraceptives (if used correctly) are very effective when it comes to preventing pregnancy. They can also be prescribed to reduce painful or heavy periods, or other conditions made worse by hormones linked to our cycle - from acne to endometriosis.
All hormonal contraceptives work by altering our bodies natural production of hormones to prevent pregnancy. This means they can also have an effect on our cycle and how we experience our periods. In some cases, hormonal contraceptives can significantly change our periods, from making them lighter and more regular, to stopping them completely. Any changes may last for a few days, weeks or months after you stop taking them.
Many hormonal contraceptives share a lot of the same advantages, disadvantages and possible side effects. But, we’re all different! Our bodies won’t all respond exactly the same way. So you might have to try a few forms of contraception until you find one that works for you and your cycle.
The combination pill or combined contraceptive pill

How it works
Combination oral contraceptive pills contain synthetic versions of the female sex hormones estrogen and progesterone. These work by suppressing ovulation, so although your uterus lining will thicken and shed every month you won’t release an egg. They also thicken the cervical mucus, making it a less friendly environment for sperm.
Designed to be taken orally at the same time every day, each sleeve contains 21 regular tablets and 7 dummy tablets. The dummy tablets allow your body to shed any uterine lining that has built up over the month. This is referred to as a withdrawal bleed, rather than a period.
You also have the option to take up to three sleeves of tablets consecutively2 (always double check with your doctor if this is ok for the type of combination pill you’re taking). So you can avoid a bleed for up to three months. This isn’t recommended to do regularly, but in some cases can be convenient - like if you’re on holiday or travelling. If you do double or treble up on packets, when you do bleed it’s likely to be heavier and possibly more painful than usual. You may also notice some breakthrough bleeding. But it is always a good idea to check with your doctor before you do this!
How effective is it?
If taken correctly, the combination pill is over 99% effective at preventing pregnancy. However, with ‘typical’ use, like Ifif you’re generally a bit disorganised and prone to forgetting to take medication, the rates drop to 93%3 meaning - this may not be the right method for you!
How it might affect your cycle
You’re likely to notice your period becomes more regular - most people experience their monthly withdrawal bleed two to three days after beginning the dummy pills at the end of a pill packet. Still having a regular bleed each month can feel reassuring for some women, as it can help you feel more in tune with your body and, of course, confirm that you’re not pregnant.
Also, as your hormones affect all kinds of things, from your appetite and mood, to energy levels and sex drive, you may be likely to notice some other changes after beginning the pill.
After stopping the pill your body should start to return to producing hormones normally. Your natural cycle should return within a few weeks to months, although you could experience other side effects like acne or reduction in breast size. This can be due to the reduction in estrogen, or just part of your body naturally adjusting - especially if you’ve been taking the pill for a long time. Importantly, taking the pill for a long time has no significant effect on fertility, and the majority of women ovulate within 3 months of stopping the pill4. If you’re worried about any symptoms or your fertility, always check with your doctor.
Let’s lay out some of the pros and cons
Some advantages of the combined pill include:
- It doesn’t interfere with sex
- Bleeding can be more regular, lighter and less painful
- It reduces your risk of cancer of the ovaries, womb and colon
- It can reduce PMS (premenstrual syndrome) symptoms
- It can reduce acne
- It may protect against pelvic inflammatory disease and the risk of fibroids, ovarian cysts and non-cancerous breast disease
- For women who don’t like the idea of not having a period, a monthly bleed can be reassuring
Disadvantages of the combined pill include:
- It can cause temporary side effects at first, or throughout use (see section below for more details on this)
- Itn can increase your blood pressure
- It doesn’t protect against STDs (sexually transmitted diseases)
- Spotting can be common in the first few months
- After stopping the pill, there can be some delay in return of your normal menstrual cycles
- It has been linked to an increased risk of blood clots5 and breast cancer6
- You could experience side effects like nausea, breast tenderness, headaches and migraines, weight gain caused by appetite changes, mood changes or a decreased libido
If you experience any of these side effects for more than a few weeks, it may just be because that particular pill isn’t right for you.
“I was on the combined contraceptive pill for 23 years. It took 6 years for me to find a pill that suited me. For me, I felt that the benefits outweigh the negatives. I experienced side effects ranging from sickness to horrendous mood swings before I found one that was right for me. I was in a long term relationship for the majority of the time and also used condoms after that ended when I had several different partners. For me, knowing that I was protected from pregnancy even if the condom split was hugely important in making the choice to stay on the pill after my relationship ended.” - Catherine, Newquay
“It seems like doctors just put you on the pill as a seemingly standard solution to every problem like PMS, pain, acne… What they don’t tell you is how much it could mess you up, even for years after coming off it. I didn’t have a proper period for two years after I stopped taking the pill.” - Alice, Bristol
“When taking the pill, my usual blemish prone /combination skin was really clear, but I had severe menstrual migraines and frequent mood swings, being overall quite irritable.” - Francesca, London
The progestogen-only pill / "mini pill"

How it works
The progestogen-only pill works by thickening cervical mucus and thinning the lining in the uterus, stopping sperm from reaching the egg. It also suppresses ovulation, but not consistently. Like the combination pill, it is likely to be taken orally at the same time every day. Each sleeve contains 28 tablets, with no dummy tablets.
How effective is it?
Over 99% effective in preventing pregnancy, if taken correctly at the same time each day.
How it might affect your cycle
Less than half of women will keep getting regular periods, , and for those whose continue, they are likely to can be lighter and less painful. Many women may have no periods at all whilst taking this type of pill, whereas some will have irregular bleeding.
Similar to the combined pill, once you stop taking the mini pill, your cycle should return to normal within a few weeks or months, and there is no long-term effect on fertility. If your periods stopped completely when taking the mini pill, they should begin again within a few weeks.
Side effects can be rarer with the progestogen-only pill compared to the combined (many women who don’t get on with the combined pill prefer the mini pill for this reason).
“I started taking the mini-pill after trying multiple combined pills and just not getting on with them. My periods stopped completely, which I was pleased about, and I didn’t get any of the unpleasant side effects like the headaches or mood swings I experienced with the combined pill.” - Alana, Portugal
“I was advised to swap from the combined pill to mini-pill due to the fact I was having frequent migraines. I found that the mini pill gave me far more regular periods and eventually my periods stopped entirely which was great!! I found that it didn't work well for me after I had a baby for some reason... the bleeding was irregular and my hormones were quite affected, so my husband decided to have a vasectomy.” - Georgia, Cornwall
Let’s lay out some of the pros and cons
Some advantages of the progestogen-only pill include:
- It doesn't interrupt sex
- You can use it when breastfeeding
- It's useful if you can't take the hormone oestrogen, which is in the combined pill, contraceptive patch and vaginal ring
- You can use it at any age – even if you smoke and are over 35
- You may notice a reduction in acne
- It can reduce or stop heavy, painful periods
Disadvantages:
- You could get spotting between periods (if you still experience periods with this type of pill)
- It doesn't protect you against STIs
- You need to remember to take it at or around the same time each day
- Some medicines, including some (uncommon) antibiotics, can make it less effective
- You may also experience other side effects like acne, breast tenderness, mood changes, headaches or migraines, nausea
- Small fluid filled cysts on ovaries may develop which are usually harmless and go away without treatment
The hormonal intrauterine system IUS (the hormonal coil)
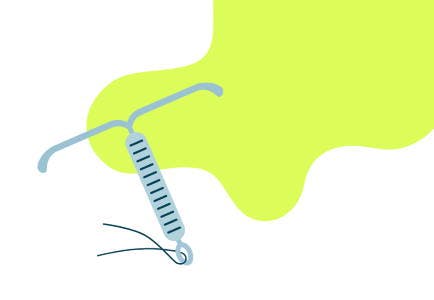
How it works
Despite the name, the IUS doesn’t really look like a coil. It’s a small, T-shaped device made of plastic that when put into the uterus, releases the hormone progestogen to prevent pregnancy. There are, in fact, two types of coils. One contains the hormone progesterone, described here, and one is made of copper, also known as the IUD which is outlined below.
The IUS prevents pregnancy by thickening the cervical mucus and thinning the lining of the womb, much like the mini-pill. It can also reduce the likelihood of ovulation occurring, but most women continue to ovulate.
Depending on the brand, it can last 3-5 years before needing to be replaced.
The Mirena coil is one of the most popular IUS devices, but there are two newer and smaller hormone coils out now, which can make them slightly easier to fit and contain lower doses of the progesterone hormone.
A GP or nurse will fit it for you, after some initial health checks (for STDs and checks on the position and size of the uterus) which takes around 20 minutes. The actual fitting of the coil only takes around 5 minutes and it is inserted through the entrance of the cervix.
You should get a check within 6 weeks after the fitting to make sure everything is fine.
How effective is it?
Over 99% effective if inserted correctly.
How it might affect your cycle
It can make your periods lighter, shorter or stop completely - which can be welcome for women who have painful or heavy periods. You might find that over time, periods become lighter and lighter and eventually stop by the first year after insertion.
Once you get an IUS removed, your periods and cycle should return to normal within a few weeks or months - and it’s also possible to get pregnant immediately.
Let’s lay out some of the pros and cons
Advantages of the IUS include:
- As it works for 3-5 years, you can “set and forget” - no needing to remember to take pills
- It doesn’t interrupt sex
- It’s safe to use if you’re breastfeeding, and can be inserted immediately after birth
- It doesn’t affect other medications
- There’s no evidence it affects weight or increases risk of cervical cancer, cancer of the uterus or ovarian cancer. It has also been shown to protect against the development of endometrial cancer.
- It’s suitable for use for any age, all the way up to menopause
- It reduces or stops heavy, painful periods
Disadvantages:
- Discomfort or pain during insertion (this should settle after insertion; if it does not the device may not be placed correctly)
- Irregular bleeding patterns – these tend to settle over time.
- Headaches, acne and breast tenderness initially, but should settle after the first 3 months of use.
- There may be changes in mood, libido and appetite
- It doesn't protect you against STIs
- Small fluid filled sacs (cysts) may develop on the ovaries but usually go away without treatment.
- Although rare, if pregnancy does occur whilst the IUS is in situ, it is more likely to be an ectopic pregnancy
- Infections may lead to a pelvic infection if not treated
- It is rare, but possible for it to come out by itself
- There is a risk of getting an infection after fitting, and for the infection to spread up the reproductive tract
“I chose a Jaydess hormone coil as it is smaller and has a lower dose of hormone. It lasts for 3 years instead of 5 like the Mirena, but I felt it was worth it as my anatomy is quite small (the doctor said there was no way I could have known this before, but I was right when they measured me!) and I wanted minimal hormones. It took a little time for my body to get used to it after the initial insertion; I had some bloating and bladder irritation, but that settled after a few weeks and I've been really happy with it ever since.
I recently had the old one removed and a new one put in, and the process was pretty simple. I can't pretend it's pain free, but it is bearable and I only had mild cramps for a couple of hours afterwards. Now I have another 3 years of no periods and not having to worry about pregnancy!
My ex said he couldn't feel the strings but a more recent partner said he could but it wasn't uncomfortable. Main pros for me: no periods and no pregnancy for at least 3 years. Main cons for me: pain of insertion, but bearable and passes quickly. Bladder irritation was annoying but did pass after a few days and I haven't had the same problem with the new one.
On balance, worth it! I appreciate others will have different views and I have heard some stories from friends (rejection where uterus has pushed it back out, ongoing cramps etc) but good to share a positive viewpoint!” - Esmé, Brighton
The 3-month shot / contraceptive injection
How it works
The hormone progesterone is given via an injection that lasts up to 13 weeks, depending on which brand is given. This is usually given by a doctor or nurse in the buttocks, but you can have it in your upper arm.
It works to suppress ovulation every month, as well as thinning the lining of the uterus so any fertilised egg is unlikely to implant. It also also thickens the cervical mucus to make it harder for sperm to move in the cervix - much like other progesterone based contraceptives.
How effective is it?
Over 99% effective if administered properly.
How it might affect your cycle
Around one in ten women stop having periods after 3 months, which goes up to 50% after a year. The longer you have consecutive injections, the more likely you are to stop having periods until you switch methods or stop having the injection.
After you’ve had the injection for the first time, it’s pretty common to experience irregular bleeding, or even heavier prolonged bleeding. This should eventually cease: if it doesn’t, speak to your doctor.
Unlike the pill, you can’t just stop the injection. Even if you decide not to renew the contraceptive injection, your regular cycle and periods may not return its regular pattern for up to a year. If you decide to try for a baby, this could have an impact on how long it takes you to conceive.
Let’s check out some of the pros and cons
Some advantages include:
- Once you’ve had the injection (as long as it’s in the first 5 days of your menstrual cycle) you’re protected immediately until it wears off. No need to remember to take a pill.
- It doesn’t interrupt sex
- It’s safe to use if you’re breastfeeding or if you’re taking other medication
- It can reduce heavy or painful periods and some symptoms of PMS
Disadvantages can include:
- It doesn’t protect you against STIs
- Once you stop taking the injection your periods might not return to normal for up to a year, which can have an effect on when you can become pregnant
- Certain brands of injection can cause weight gain
- Headaches, acne, decreased libido, mood swings or hair loss may increase
- Side effects may continue until the injection wears off, and for some time afterwards until it completely leaves your system.
“For about 7 years before I fell pregnant, I was on the injection. It worked wonders for me. No periods, no symptoms and no mood swings (as far as I’m aware). Prior to that I was on the progestogen only pill because I suffered from migraines (the one without a break). It was awful, massive weight gain and totally irregular periods, worse than my usual periods which were extremely heavy and never regular.
When I knew we were going to try for a baby, I came off the injection in March, went straight onto the pill until July and fell pregnant in September! 4 months after giving birth when I had stopped breast feeding, I have the mirena coil. Occasionally I get very light bleeding, with some cramping even when I don’t bleed, I can actually feel myself ovulating too but apparently that’s common after giving birth regardless of what contraception you go on. A year on and that’s working well for me too!” - Charlie, Bournemouth
“The injection was sold to me as my best option when I was 19. During my time on the injection which I had three times over 9 months, I gained over a stone in weight, I became clinically depressed, my periods completely stopped for two years and I lost my sex drive totally. I didn’t even want to be touched. After the third time getting the injection I immediately threw up. It took me years to get my periods back into a regular cycle. I instinctively knew the injection was bad for me and my body, although I was told repeatedly my symptoms had nothing to do with the contraceptive injection.” - Miranda, London
The implant

How it works
A small cylindrical flexible plastic implant is placed just under the skin in your upper arm by a nurse or doctor. The process is a bit like having an injection. It releases progesterone into your bloodstream gradually, to prevent pregnancy for up to 3 years. It’s main mode of action is by preventing ovulation, but it can also thicken the cervical mucus preventing sperm from swimming easily, and by thinning the lining of the womb to stop implantation.
How effective is it?
The implant is more than 99% effective.
How it might affect your cycle
The implant usually makes periods lighter and less frequent, or your periods can stop altogether. It can also make periods less painful if you suffer from bad cramping. However it is important to note that some people can find they have irregular spotting or heavier, more prolonged bleeding than before.
As soon as you have the implant removed, you’re no longer protected against getting pregnant. But it could still take a little while for your regular cycle to return to normal again.
Let’s check out some of the pros and cons
Some of the advantages are:
- It doesn’t interrupt sex
- It lasts for up to three years so you don’t have to remember to take a pill each day
- You can have it taken out immediately if you get any side effects
- It’s safe to use when breastfeeding
- It could help to relieve heavy or painful periods
Disadvantages are:
- It doesn’t protect against STIs
- If you have it removed, some side effects may not stop immediately
- The area where the implant is inserted can be a little sore or feel bruised at first
- You may start getting acne, or existing acne could get worse
- You may experience nausea, sore breasts, mood swings and weight gain or appetite changes
- Some studies have found that it can also decrease sex drive, which can be a cause to discontinue with the implant
The patch

How it works
This small patch is stuck onto your skin and releases progestin and estrogen - the same hormones as the combined pill - to prevent pregnancy. It does this by stopping ovulation, thickening the cervical mucus to make it hard for sperm to mobilise through the cervix. Another effect is that it can thin the lining of the uterus (womb), preventing a fertilized egg from implanting.
Every patch lasts one week (7 days), so you can replace the patch each week for three weeks running and on the fourth week take a break. The fourth week is when you experience your withdrawal bleed, although not everyone will have one of these.
The patch is pretty hardy and waterproof, so you can go about any of your regular activities whilst using it. You can stick it pretty much anywhere but on smoother skin, or where it’s not likely to get rubbed off by tight clothing, is best.
How effective is it?
The patch is more than 99% effective if used properly and replaced regularly.
How it might affect your cycle
The patch might make your monthly bleed lighter, more predictable and less painful. Your periods may stop altogether whilst you’re using it.
Let’s check out some of the pros and cons
Some of the advantages are:
- It doesn’t interrupt sex
- It’s really easy to use
- It can help with PMS symptoms
- It still works if you vomit or have diarrhoea
- You don’t have to remember to take a pill every day, just to replace your patch once per week
- If you decide not to continue, you can take off your patch the same day
The disadvantages can be:
- It doesn’t protect against STDs
- Although the patch is pretty secure if it’s well placed, it is possible for it to come off accidentally
- It’s visible unless covered with clothing
- It can cause skin irritation, itching or soreness
- Some medicines can make it less effective
- It may not be suitable for breastfeeding
- They can increase the possibility of blood clots - so if you’ve had one before or are more at risk, the patch may not be right for you
The vaginal ring (the NuvaRing)

How it works
The vaginal ring is a small, soft, flexible ring made from plastic that is designed to be placed inside the vagina. You leave it in for 21 days at a time, removing it for 7 days at the end of your cycle to induce allow a withdrawal bleed (not everyone will experience a withdrawal bleed).
It releases a steady dose of the hormones oestrogen and progestin into the bloodstream to prevent pregnancy4. Like other forms of contraception with oestrogen and progestin, it works by inhibiting ovulation, thickening cervical mucus and thinning the lining of the womb to prevent implantation.
How effective is it?
If used correctly, the vaginal ring is over 99% effective at preventing pregnancy.
How it might affect your cycle
As the ring inhibits ovulation, your monthly bleed will be a withdrawal bleed rather than a regular period. This will mean it will probably be lighter and less painful than usual, or you may not have one at all.
Let’s check out some of the pros and cons
Some of the advantages are:
- It doesn’t interrupt sex (you can have sex and use tampons whilst using it)
- It lasts for a month so you don’t have to think about it every day
- There is no long term effect on your fertility
- It can help reduce PMS symptoms
- It can potentially reduce the risk of some cancers
- The addition of oestrogen can help with issues such as acne and PMS symptoms
Disadvantages are:
- It doesn’t protect against STIs
- You have to remember to remove it after 21 days and replace 7 days later
- Some medicines can make it less effective
- It can cause side effects such as headaches or migraines, nausea, breast tenderness and mood changes.
- It can increase the risk of blood clots, although this is rare
- You might not like the feeling of inserting or removing it
- You may not like the feeling of it during sex - if you can feel it at all
Emergency contraceptive (the “morning after” pill)

Although you can also get the copper IUD inserted as a form of emergency contraception, here we are focussing specifically on the medical forms of emergency contraception, known as the 'morning-after’ pill.
How it works
The emergency contraceptive is designed - you may have guessed - for use in emergencies! Not as a planned, or regular form of contraception.
It comes in pill form (either one or two pills, depending on the brand) and you take it as soon as possible after having unprotected sex to prevent pregnancy.
It releases hormones to prevent pregnancy - most contain levonorgestrel, a synthetic version of progesterone.
How effective is it?
If you need to take the morning after pill you should do it as soon as possible. How well pregnancy can be prevented will depend on where you are in your menstrual cycle, because unprotected sex during the fertile window will carry the highest likelihood of resulting in pregnancy. It is recommended that you take it within 24 hours, but if you take it within 72 hours there’s just a 1-2% chance of getting pregnant overall.
This is because the emergency contraceptive is designed to block pregnancy by preventing the release of an egg so it cannot be fertilized. If you’re already pregnant, this pill won’t work as a contraceptive.
How it might affect your cycle
It can make your next period heavier, earlier or later. If your period is more than seven days late you’ll need to take a pregnancy test.
Let’s check out some of the pros and cons
The advantages are:
- If you don’t wish to conceive but weren’t protected during sex, it’s a very effective way of preventing pregnancy
- It’s easy to obtain from most chemists if you can’t get an immediate appointment with your doctor
- It’s safe to use when breastfeeding
Disadvantages are:
- It can make your next period heavier or more painful
- It doesn’t protect against STDs
- It's less effective the larger longer the time gap between having sex and taking the pill
- It’s only designed for emergencies, and will not always prevent pregnancy if conception has already occurred
- Although easy to obtain, it can be expensive
Non hormonal contraceptives
Sometimes hormonal contraceptives aren’t suitable. This can be for all kinds of reasons, from health to lifestyle.
It’s true that non-hormonal methods might not have some of the practical advantages of hormonal methods. And they often require more planning and thought. But they also don’t have many of the disadvantages or side effects that some people experience using hormonal contraceptives. They also don’t affect your natural hormonal cycle in the same way - which allows your body to just do its thing without interference.
Intrauterine device IUD / "copper coil"
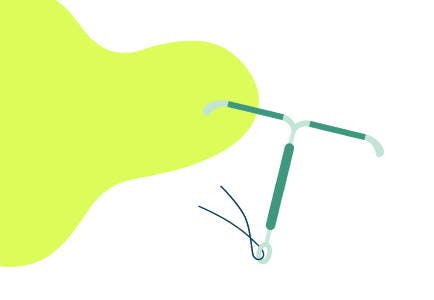
How it works
The coil gets its name from the fine coil of copper that surrounds part of this small T-shaped device. It’s placed through your vagina by a nurse or doctor, and sits in the neck of the womb where it gradually releases copper to stop pregnancy.
Due to the presence of copper ions in the uterus, the coil creates an inflammatory response which prevents sperm from reaching the egg to fertilise it.
How effective is it?
When inserted correctly it’s more than 99% effective and it lasts for 5-10 years.
How it might affect your cycle
Your periods can become longer, heavier and more painful. This isn’t ideal if you already struggle with heavy periods. However this effect may gradually settle over time after the first 6 months.
Because there are no added hormones it shouldn’t cause any changes to your moods, headaches, migraines or increase breast tenderness.
Let’s check out some of the pros and cons
Some of the advantages are:
- It works immediately after insertion
- It’s over 99% effective
- It lasts for 5-10 years before it needs removing
- There are no hormonal side effects
- It doesn’t interrupt sex
- It’s safe to use when breastfeeding
The disadvantages are:
- It doesn’t protects against STDs
- It can cause heavier, more painful periods temporarily
- It can be painful when first inserted
- Infections can lead to pelvic infections when not treated (there’s a small chance of pelvic infection in the first 20 days after an IUD is inserted)
- It can cause thrush, or repeated thrush infections
- It can be rejected and expelled by the body
- It can move after it’s been inserted
- In rare cases, insertion can cause damage to the womb
Condoms (for men)

How they work
Condoms are usually made of stretchy latex (although they’re also available in materials suitable for people with latex allergies). They’re designed to be rolled onto an erect penis by pinching the tip of the condom (leaving some space at the top for semen) and rolling it down towards the base of the penis until it stays in place securely.
After ejaculation the condom should be securely held at the base before withdrawing the penis from the vagina.
Condoms are single use, and should be disposed of in a bin (not a toilet). Only buy condoms with the CE mark or BSI Kitemark on the packet. This shows they’ve been tested to the highest safety standards. It’s also a little known fact that condoms have an expiry date, so make sure you check yours is in date!
How effective is it?
98% effective when used correctly.
How it might affect your cycle
Condoms don’t affect your hormones in any way, so your natural cycle should continue unchanged.
Let’s check out some of the pros and cons
The advantages are:
- They protect you against STDs
- They’re 98% effective
- They don’t affect your natural hormone cycle
- You don’t need a prescription for them
- The lubricated coating on condoms can make sex more comfortable for some women
- There’s wide variety of different types of condoms to choose from
- Safe to use when breastfeeding
Disadvantages can be:
- They can interrupt sex
- Some people find they make sex less pleasurable
- Some people find them uncomfortable
- Unless obtained from a free provider such as the NHS, they can be expensive
- They can break or slip
- You need to remember to have some handy
Condoms (for women)

Although not as popular as the male condom, you can also get condoms for women. Designed to be fitted inside the vagina before sex, they are clear latex tubes that look similar to a large, unrolled male condom.
Let’s check out some of the pros and cons
The advantages are:
- They help protect you against STDs
- They’re 95% effective when used correctly
- They don’t affect your natural hormone cycle
- You don’t need a prescription for them
- They’re safe to use when breastfeeding
Disadvantages can be:
- They can interrupt sex
- Some people find they make sex less pleasurable
- Some people find them uncomfortable
- Unless obtained from a free provider such as the NHS, they can be expensive and not as widely available as male condoms
- You need to remember to have some handy
Cervical cap or diaphragm

How it works
It’s a small semi circular shaped cap made of soft, flexible silicone that fits below the cervix to stop sperm entering. It only works if you also use it with spermicide.
It needs to be left in place for at least 6 hours after sex. You can insert it into the vagina yourself, but it may take some practice.
How effective is it?
When used correctly with spermicide, it’s 92-98% effective.
How it might affect your cycle
It won’t affect your regular cycle at all.
Let’s check out some of the pros and cons
Some of the advantages are:
- It’s 92-98% effective
- It doesn’t affect your natural cycle as there are no added hormones
- You can insert and remove it yourself
- It’s safe to use when breastfeeding
- There are no serious health risks
- There are different size caps available
Some of the disadvantages are:
- It doesn’t protect against STDs
- It may interrupt sex
- If it has been in place more than 3 hours you need to add more spermicide
- It can cause cystitis
- It can take a bit of practice to insert correctly (and you have to remember to remove it)
Pull out method

How it works
This is where a man would withdraw his penis from a woman's vagina before he ejaculates. Instead of ejaculating inside her vagina during intercourse.
How effective is it?
Around 78% effective. On average, out of 100 couples using the withdrawal method, 22 will get pregnant within a year. That’s around one in five.
As sperm can be released from the penis before ejaculation (in a substance called pre-ejaculation) even if the withdrawal method is used correctly every single time, there’s still a higher chance that you can fall pregnant than if you use other forms of contraception.
Generally this method shouldn’t be used if you definitely don’t want to get pregnant.
How it might affect your cycle
The withdrawal method doesn’t affect your hormones in any way, so your natural cycle should continue unchanged.
Let’s check out some of the pros and cons
Some of the advantages are:
- It doesn’t affect your hormones and natural cycle
- You don’t have to see a doctor for a prescription or procedure
- It’s safe to use when breastfeeding
Disadvantages are:
- It can interrupt sex
- It doesn’t protect against STDs
- It can be hard for a man to control
- A woman has no control over it
- High rate of unintended pregnancy
Rhythm method, with temperature monitoring

How it works
This involves only having sex on certain days of the month when fertility is low - or using alternative contraception on those days. Fertility is monitored using basal body temperature readings alongside charting your monthly cycle in a calendar and inputting other information such as cervical secretions. Basal body temperature (if taken extremely accurately) can help determine when a woman is ovulating. This is because temperature is higher on ovulation days.
This method can also be used alongside ovulation kits which measure levels of hormone in the urine. You can also chart observed changes in cervical mucus which can help to indicate fertility levels during the month. As the temperature rises, a date is calculated for predicted ovulation. No additional contraceptive precautions are required for sex that has occurred from 3 days after the temperature rise until the start of menstruation. In women wishing to avoid a pregnancy, avoidance of sex, or use of additional contraceptive precautions, is then required until higher temperatures have again been recorded on three consecutive days in the next cycle.
As a woman is only fertile for a certain amount of days per month, (before, during and immediately after ovulation) the rhythm method is designed to help avoid having sex during this fertile period. This is why this method is best for people only with an extremely regular menstrual cycle.
How effective is it?
This can depend. Because sperm can survive in the reproductive tract for five to seven days, you can still get pregnant even if you have sex several days before ovulation or some days afterwards.
Also, for most women it’s very difficult to determine when the safe times to have sex are. This is because ovulation isn’t always regular and varies between women. A very accurate thermometer and method of temperature taking is needed for taking basal rates. And it can mean up to 10 or more days of abstinence (or alternative contraception methods) per month.
The rhythm method is around 80-87% effective at preventing pregnancy, but only when used accurately. So, it may not be the best method to use by itself if you definitely don’t want to fall pregnant.14
How it might affect your cycle
This method doesn’t affect your natural cycle at all, and can help you get to know your body better.
Let’s check out some of the pros and cons
Some of the advantages are:
- It doesn’t interrupt sex
- It doesn’t affect your hormones and natural cycle
- It doesn’t affect any medication you’re currently taking
- It can help you understand your natural cycles and body better
Disadvantages are:
- It is one of the least effective methods of birth control due to the difficulty of using it accurately
- It doesn’t protect against STDs
- On higher risk days alternative protection against pregnancy should be used
“I use the rhythm method now after having been on the combined pill for 13 years. I much prefer it to the pill, but you have to be much more careful. I’m also in a committed relationship so if I did get pregnant it wouldn’t be a disaster, although I don’t feel ready to yet! I just prefer how my body is when I’m not taking additional hormones. Periods are more painful, but I feel like it’s the best decision for me.” - Katherine, Scotland
“I used the rhythm method with the aid of an app, but without using temperature monitoring when I was actually trying to get pregnant after coming off the mini-pill. After around seven months, when I used a digital ovulation test, I found that I was ovulating at a completely different time to what I thought - and what the app was telling me. Once I knew when I was ovulating I became pregnant right away. This made me realise if I’d been trying to avoid getting pregnant, this app would definitely NOT have worked since I ovulated on what it told me were “low risk” days! Just goes to show you definitely can’t trust an app on its own.” - Carly, Leeds
Key takeaways
There is no right or wrong choice when it comes to contraception. It’s a personal choice that depends on your individual body and circumstances.
It’s also impossible how to tell, beforehand, how your body will adapt to most contraception methods. Some people find one that works for them right away. But many women have to try a few different methods before settling on one they’re comfortable with.
Whichever methods of contraception you choose, no form of contraception is 100% effective, but as long as you’re using it correctly, in most cases there’s only an extremely low chance that you’ll become pregnant.
The best way to make an initial decision is based on the information you’ve researched and advice from your GP or sexual health clinic.
References
1. Baird DT, Glasier AF. Hormonal Contraception. N Engl J Med 1993; 328: 1543–1549.
2. Wright KP, Johnson J V. Evaluation of extended and continuous use oral contraceptives. Ther Clin Risk Manag 2008; 4: 905–911.
3. Trussell J. Contraceptive failure in the United States. Contraception 2011; 83: 397–404.
4. Faculty of Sexual and Reproductive Healthcare. Clinical Guidance: Combined Hormonal Contraception. BMJ Sex Reprod Heal 2019; 45: 1–93.
5. Lidegaard Ø, Løkkegaard E, Jensen A, et al. Thrombotic Stroke and Myocardial Infarction with Hormonal Contraception. N Engl J Med 2012; 366: 2257–2266.
6. Mørch LS, Skovlund CW, Hannaford PC, et al. Contemporary Hormonal Contraception and the Risk of Breast Cancer. N Engl J Med 2017; 377: 2228–2239.
7. Faculty of Sexual and Reproductive Healthcare (FSRH). Clinical Guidance: Progestogen-only pills. FSRH Clin Guidel; 2015 https://www.fsrh.org/standards-and-guidance/documents/cec-ceu-guidance-pop-mar-2015/ (2019).
8. Faculty of Sexual and Reproductive Healthcare. Clinical Guidance: Intrauterine Contraception. Fac Sex Reprod Healthc 2015; 2015: 19.
9. Faculty of Sexual & Reproductive Healthcare. Clinical Guidance: Progestogen-only Injectable Contraception. 2014 https://www.fsrh.org/standards-and-guidance/documents/cec-ceu-guidance-injectables-dec-2014/ (2020).
10. Faculty of Sexual & Reproductive Healthcare. Clinical Guidance: Progestogen-only Implants. Fac Sex Reprod Healthc 2014; 1–32.
11. Boozalis A, Tutlam NT, Chrisman Robbins C, et al. Sexual Desire and Hormonal Contraception. Obstet Gynecol 2016; 127: 563–572.
12. Faculty of Sexual and Reproductive Healthcare (FSRH). Clinical Guidance: Emergency contraception. 2017; 2017: 57.
13. Faculty of Sexual & Reproductive Healthcare .Clinical Guidance: Barrier Methods for Contraception and STI Prevention. Fac Sex Reprod Healthc Clin Guid; 2012 https://www.fsrh.org/documents/cec-ceu-guidance-barriers-aug-2012/cec-ceu-guidance-barriers-aug-2012.pdf (2015).
14. Faculty of Sexual and Reproductive Healthcare (FSRH). Clinical Guidance: Fertility Awareness Methods. 2015 https://www.fsrh.org/standards-and-guidance/documents/ceuguidancefertilityawarenessmethods/ (2015).
Section jump
Back to top